Can your baby breathe all through the night? Can he nap without life support? Does her little body do the involuntary things necessary to survive sleep? I pray that it’s so for you.
It’s not like that for Ian.
This dapper little dude with the baby blue eyes, the flirty smile and the permanent tracheostomy, has Congenital Central Hypoventilation Syndrome (CCHS). In short, you have something he doesn’t – a part of your brain that senses rising carbon dioxide levels in your blood and tells you to breathe. Out with the bad (CO2), in with the good (O2). When you sleep, it’s this particular part of your noggin that keeps you breathing.
Ian’s doesn’t work.
When Ian sleeps, his whole brain sleeps, including the critically important part that tells the lungs to breathe. Ian dies in his sleep every night. Only one thing lets him wake up each morning – his mother’s commitment to putting him on a ventilator. Every night. Every nap. Without fail.

When Ian was born, his parents were mysteriously absent from social media. Though we’d been longtime friends, I’m embarrassed to say our daily lives distracted us from the fact that there were no typical baby updates, no proud pictures, no milestones being shared. Honestly, we just didn’t notice. Six months later we learned why – they had endured a living nightmare and had spent months literally just trying to survive. Once they came up for air, the rest of us were shell shocked.
There was an Oscar-nominated documentary released last year called, “Our Curse”. If you can watch it without crying I’m not sure we can be friends. I don’t care if you know these families or not, it’ll tear your heart right out. It’s an authentic, almost voyeuristic look inside the home of a CCHS baby. And our friends were living it.

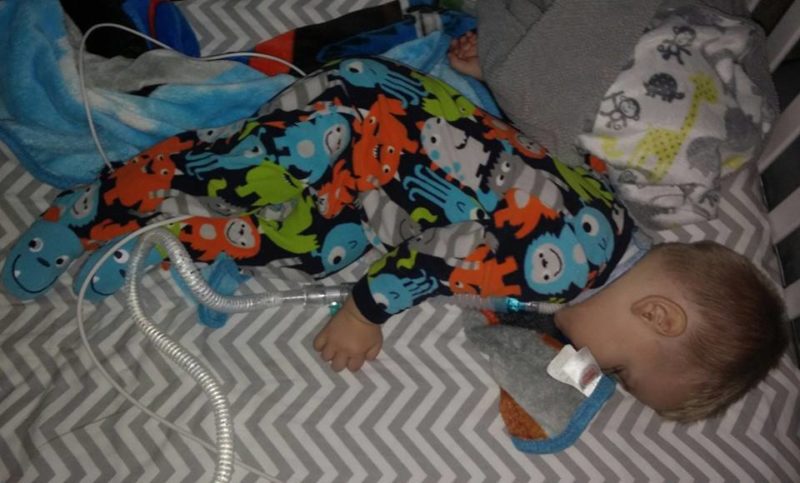
I’ve met Ian. I’ve heard his giggle. I can only imagine the way his father’s heart shatters when his trach is out and no sound emerges when Ian laughs or cries. We’ve watched him play with our children. We see how vigilant his parents must be to ensure he’s not getting tired without his ventilator nearby. We’ve watched him sleep. I was given the honor of sneaking into his room one night. My fingers fail on this keyboard to convey the gravity of that moment.
To hear the hiss of the ventilator, see the green glow of the monitors, marvel at the tangle of tubes going into the crib, and listen as my friend explained the numbers I was seeing.
The number of breaths he’s taking by himself.
Zero. He’s not breathing.
This child I spent the day with is on life support. And tomorrow I will have breakfast with him.
The brain of this mama could hardly cope to just be near it, just to know it. But his mama. Wow. How? How does she do it? Like a freaking superhero is how. I’m proud of myself for getting my kid to volleyball practice on time, for getting dinner on the table, for raising polite kids. But here’s a completely average day for Ian’s mom:
- Do all the things a normal toddler mom has to do.
- Recognize any signs that he’s getting drowsy and get him hooked up to the ventilator.
- Be sure to always have a travel ventilator; he must be hooked up in the car. Kids nap in cars. Remember Ian the next time your kid spills a juice box on the road or gets hold of a rogue Sharpie in the back seat. Recently, Ian accidentally pulled out his ventilator while at a stop light. His mom had to throw it in park, climb over the seat, connect her kid back to the breath of life itself, and buckle back up before the light changed. True story.

- Clean his nebulizers and trach every morning & every night. Weekly replace his trach and sterilize the old one, change out his ventilator circuit (tubing) and all other equipment (suction tubing & canisters, humidifier chamber, pulse oximeter sensor).

This crib-side cart is where the critical magic happens - Keep his house as clean as a hospital. Seriously, this little dude can’t afford to get sick. There’s a sign on the door that lovingly advises all potential visitors to turn around and leave if they aren’t healthy themselves.
- Battle the insurance company. Twice the insurance company has denied their claim for tracheostomy tubes and supplies. TWICE! They say it’s not “medically necessary”. I can’t even type more on this bullet point without losing my composure.
- Scour the internet for other CCHS families to connect with, and even to barter supplies with. These supplies are frequently on back order. What if there were no more Epi-Pens available for kids with allergies? The only supply in existence is already owned by other allergy moms around the country. What would you do to secure them? Would you share? Would anyone else? Insert inhalers, seizure medication, etc. and a lot of people can relate. But can we really? Most of these things are for use in the event of an emergency. A device you need just in case. But Ian needs it by nightfall.

What’s in YOUR linen closet? - Look for creative ideas to disguise the permanent capped trach in the front of his throat, ways to insulate his tubing, ways to secure various equipment to the crib at the right angle.

- Never sleep again. Like forever and ever. You thought listening for your newborn’s cries was bad. Maybe you even crept in to check on them from time to time to be sure they were breathing. But in your heart of hearts, you knew the chances were good that they were. Such chances don’t exist at Ian’s house. He pulls out his tube, he pulls off his oxygen monitor, his hoses get wrapped around him or kinked up. The list of things that will go fine is shorter than the list of what can go tragically wrong. And you can’t bump the hubby with your elbow because it’s his turn to deal with the baby. You can’t yawn and stretch and shuffle over there groggily. His next breath is waiting on you, sleepy mama bear. Beeps, whirs, alarms. All night. Every night.
And not just for the baby years. Not just for the toddler years. For all the years.
There is currently no cure for CCHS. The only treatment is artificial ventilation. The battle is forever. Ian’s mom shares stories all too often of adults with CCHS who doze off without their vent. Young moms with this condition that don’t survive their child’s early days, because aren’t we all so very, very tired as new moms? They get sleep deprived like the rest of us and sit down for just a minute to close their eyes…
There’s no cure and very little awareness. This is why I write such a difficult piece. Believe it or not, we know two families with CCHS kiddos. With under 500 known cases in the US (1,200 around the world), what are the chances we’d meet 2 in different circles of life? We are the exception, though. Most people have never heard of this condition. The attention isn’t there; so the money isn’t there. We’ll never make it to the finish line with a cure if we are too poor to start the race.
This is where you can help – cash and sharing. If you can contribute to the cause, please do. If not, then share this article. Bring awareness to the need. We need to bring these patients into the light and give them hope for the future.
To learn more about Ian’s individual journey, follow him on Facebook here: Ian’s Story.
If you feel moved to join the fight for Ian and kids like him, please consider donating to The CCHS Foundation.
The CCHS Family Network is a great resource for education about this community.
Tonight, as you listen to your little people softly breathing in their sleep, thank your lucky stars. And say a prayer for CCHS warriors around the country who won’t be sleeping at all so that their little ones can.